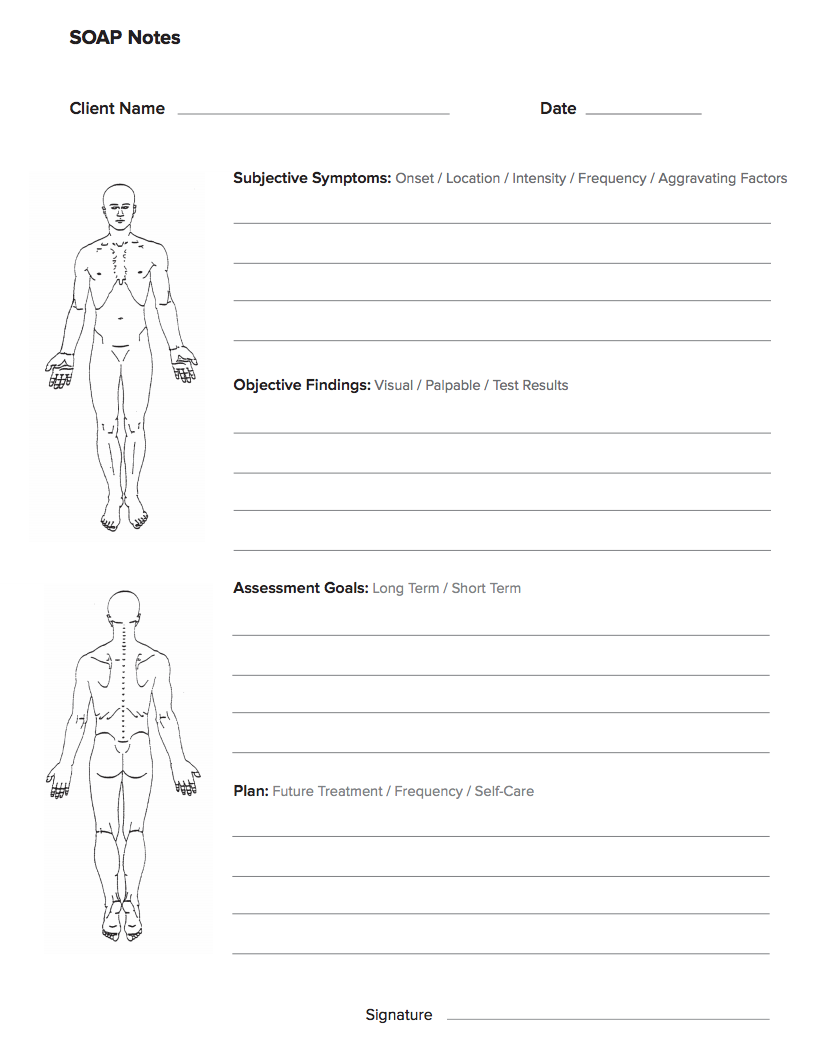
40 Fantastic Soap Note Examples Templates Templatelab
The soap note stands for subjective, objective, assessment, and plan. this note is widely used in medical industry. doctors and nurses use soap note to document and record the patient’s condition and status. the soap note is considered as the most effective and standard documentation used in the medical industry along with the progress note. Creating a record of detailed treatment notes allows a medical professional to build their own mini-research library. you will note what works, what doesn’t and everything in between. writing great physical therapist soap notes is a tried and true method for collecting data.
Patient Medical Records Johns Hopkins Medicine
Documenting a patient assessment in the notes is something all medical students need to practice. this guide discusses the soap framework (subjective, objective, assessment, plan), which should help you structure your documentation in a clear and consistent manner. you might also find our other documentation guides helpful. Soap notes (subjective, objective, assessment, plan) although only one component of the entire pomr have become the standard in clinical record keeping for daily chart notes in ambulatory settings. and google play), to record the miles traveled, record your routes and document your adventures you can even participate in challenges against other skaters leafboard is also another quite worthy scooter, if what you are looking for is an economic and solid model boosted 2 dual + ($ 1,500) in addition to
How To Write A Soap Note With Pictures Wikihow
Confidential patient medical records are protected by our soap model for medical records privacy guidelines. patients or representatives with power of attorney can authorize release of these documents. we are experiencing extremely high call volume related to covid-19 va. Electronic medical record implementation will allow your health records to be in one digital file. learn about electronic medical record implementation. advertisement schoolchildren in the united states are often threatened with an ominous-. Template for clinical soap note format. subjective the “history” section. hpi: include symptom dimensions, chronological narrative of patient’s complains, information obtained from other sources (always identify source if not the patient). pertinent past medical history. Until she married musician nick cave, she was susie bick, the 90s model discovered by photographer that saw her on the cover of two roxy music records, shot for ad campaigns, including yves.
Chart providing details of maine medical records laws internet explorer 11 is no longer supported. we recommend using google chrome, firefox, or microsoft edge. are you a legal professional? visit our professional site » created by findlaw'. A soap note, or a subjective, objective, assessment, and plan note, contains information about a patient that can be passed on to other healthcare professionals. to write a soap note, start with a section that outlines the patient's symptoms and medical history, which will be the subjective portion of the note. Soap notes an acronym for subjective, objective, assessment and plan is the most common method of documentation used by providers to input notes into patients’ medical records. they allow providers to record and share information in a universal, systematic and easy to read format.
How Is The U S Implementing Electronic Medical Records Howstuffworks
The very first soap note template was created and developed by a brilliant doctor named lawrence weed way back in the 1960s. it was done at the university of vermont as an element of the pomr (problem-oriented medical record). during those times, objective documentation did not exist so physicians had the tendency to make decisions about. The problem oriented medical record and the “academic” soap the goals of the problem oriented medical record (pomr): the pomr is an instructional tool for teaching both medicine and clinical problem solving skills. it is also a useful template for writing medical records for any case that has more than one major problem. Developed by dr/ lawrence weed in the 1960s, the soap note template methodology records vital patient medical information, to provide evidence of patient contact, and to inform a clinical reasoning process. soap notes have four main parts, designed to help improve evaluations and standardize documentation: subjective what the patient tells you. soap model for medical records Soap or soap notes as they are widely called also find extensive usage in veterinary practices. it is a way for clinics to record, document, and store patient’s medical information in a systematic way. it also gives the practice a framework to evaluate information without losing even the tiniest bit.
State Medical Records Laws Findlaw
A hacker claims to have stolen just shy of 10 million records, and is putting them on for sale on the dark web for about $820,000. the hacker posted the records on the site therealdeal, and the data includes social security numbers, address. A brief overview of documenting patient reviews using the soap structure soap model for medical records (subjective, objective, assessment, plan). clinical examination a comprehensive collection of clinical examination osce guides that include step-by-step images of key steps, video demonstrations and pdf mark schemes. The soap note (an acronym for subjective, objective, assessment, and plan) is a method of documentation employed by healthcare providers to write out notes in a patient's chart, along with other common formats, such as the admission note. documenting patient encounters in the medical record is an integral part of practice workflow starting with appointment scheduling, patient check-in and exam.

A soap (subjective, objective, assessment, plan) note is a method of documentation used specifically by healthcare providers. soap notes are used so staff can write down critical information concerning a patient in a clear, organized, and quick way. soap notes, once written, are most commonly found in a patient’s chart or electronic medical records. Soap notes are a highly structured format for documenting the progress of a patient during treatment and is only one of many possible formats that could be used by a health professional[1]. they are entered in the patients medical record by healthcare professionals to communicate information to other providers of care, to provide evidence of patient contact and to inform the clinical reasoning process. Soap notes are a highly structured format for documenting the progress of a patient during treatment and is only one of many possible formats that could be used by a health professional[1]. they are entered in the patients medical record by healthcare professionals to communicate information to other providers of care, to provide evidence of patient contact and to inform the clinical reasoning. 2. soap note for counseling sessions (pdf). 3. soap note for coaching sessions (pdf). a take-home message. whether you are in the medical, therapy, counseling, or coaching profession, soap model for medical records soap notes are an excellent way to document interactions with patients or clients. soap notes are easy to use and designed to communicate the most relevant information about the individual.

Components. the four components of a soap note are subjective, objective, assessment, and plan. the length and focus of each component of a soap note vary depending on the specialty; for instance, a surgical soap note is likely to be much briefer than a medical soap note, and will focus on issues that relate to post-surgical status. Whether you're interested in reviewing information doctors have collected about you or you need to verify a specific component of a past treatment, it can be important to gain access to your medical records online. this guide shows you how. An “academic” soap is different from how you will soap cases in private practice! (some different goals) there is. no. one right way to write a soap or soap a case. there will be different expectations from different clinicians and different clinical services. (sa referral is our model) it takes practice! (and time). Shown above is an example of a medical soap note that discusses the present state of a patient who came to the clinic to seek answers for a few complaints. practitioners tend to go into detail with their analysis to gather a sufficient amount of information for their records. 6. nutrition medical soap note.
Each time you hop up on a doctor's exam table, somebody makes a note in your medical records. there may come a time when you need your medical information, so find out how to get it and how it's protected. each time you climb up on a doctor. The soap format is a way for medical professionals to provide a clear, concise documentation of a client's care. it is used by a soap model for medical records variety of providers, including doctors, nurses, emts and mental health providers. soap format is intended to examine a patient's well-being and progress from several perspectives, ultimately providing him with the.